Video: https://youtu.be/F96UhMM4dxo
The information of this blog is based on our own research, with which AI then generated a video and voice-over for.
We have had an expert from medical interpretation services to review it.
This is an interesting look at what AI generates when given human input.
For example, it starts the video by asking the question: “Am I the only one who didn’t know the true weight of medical interpreters?”
And then it asks other questions like what it thinks patients will hear: “Can I afford this?” and “Will it hurt?”
These are questions that the AI came up with on its own while the rest of the content after that is what we input into the prompt.
We also included data from various sources such as a 2023 article from Palliative Medicine.
Researching data and having AI help to put it together into an emotional video really helps to show our point about how important interpreters are and what they carry on their shoulders. They are truly so important to our lives!
Transcript
Am I the only one that didn’t know the true weight of medical interpreters? These unsung heroes are more than just translators.
Imagine you’re in a hospital room, a patient gasps for air, the doctor explains three life altering options, and the interpreter, they’re the only one who truly understands both sides. Medical Interpreters face immense challenges. They hear questions like, can we afford this or will it hurt? They must navigate these with precision, staying objective, not swaying decisions.
Studies show even a minor translation slip can impact choices. They’re not just wordsmiths. They’re crucial mediators. Did you know interpreters often experience distress, overwhelm, guilt, loneliness and discomfort?
When facilitating palliative care conversations, “76% of interpreters found end of life conversations more stressful than others” [The emotional effects on professional interpreters of interpreting palliative care conversations for adult patients: A rapid review. Palliat Med. 2023].
They need our support, debriefing, mental health resources, because their role is more vital than we realize.
Next time you’re at a hospital, remember interpreters are the fragile bridge between fear and clarity; science and the human heart. Let’s support them as they support us.
Visual Storytelling
We provided our content to AI and let the AI work its magic. Here’s how the transformation unfolded:
- Script Adaptation: AI transformed the blog into a script while maintaining the emotional depth of the narrative. AI’s understanding of context ensured key moments, like the patient gasping for air or the interpreter navigating life-or-death translations, were vividly demonstrated.
- Scene Composition: AI automatically selected visuals that resonated with the content. Sterile hospital rooms, moments of intense decision-making, and the emotional toll of interpreters.
- Audio Enhancements: Voiceovers and background music were added to match the video’s tone.
After uploading the script into AI, we selected:
- Platform: “YouTube” (serious tone, fitting for healthcare content).
- Voiceover: A professional, empathetic narrator (AI-generated).
- Audience: General public
- Duration: 2 minutes
The AI synced visuals to the script, adding captions and transitions where needed.
The Result
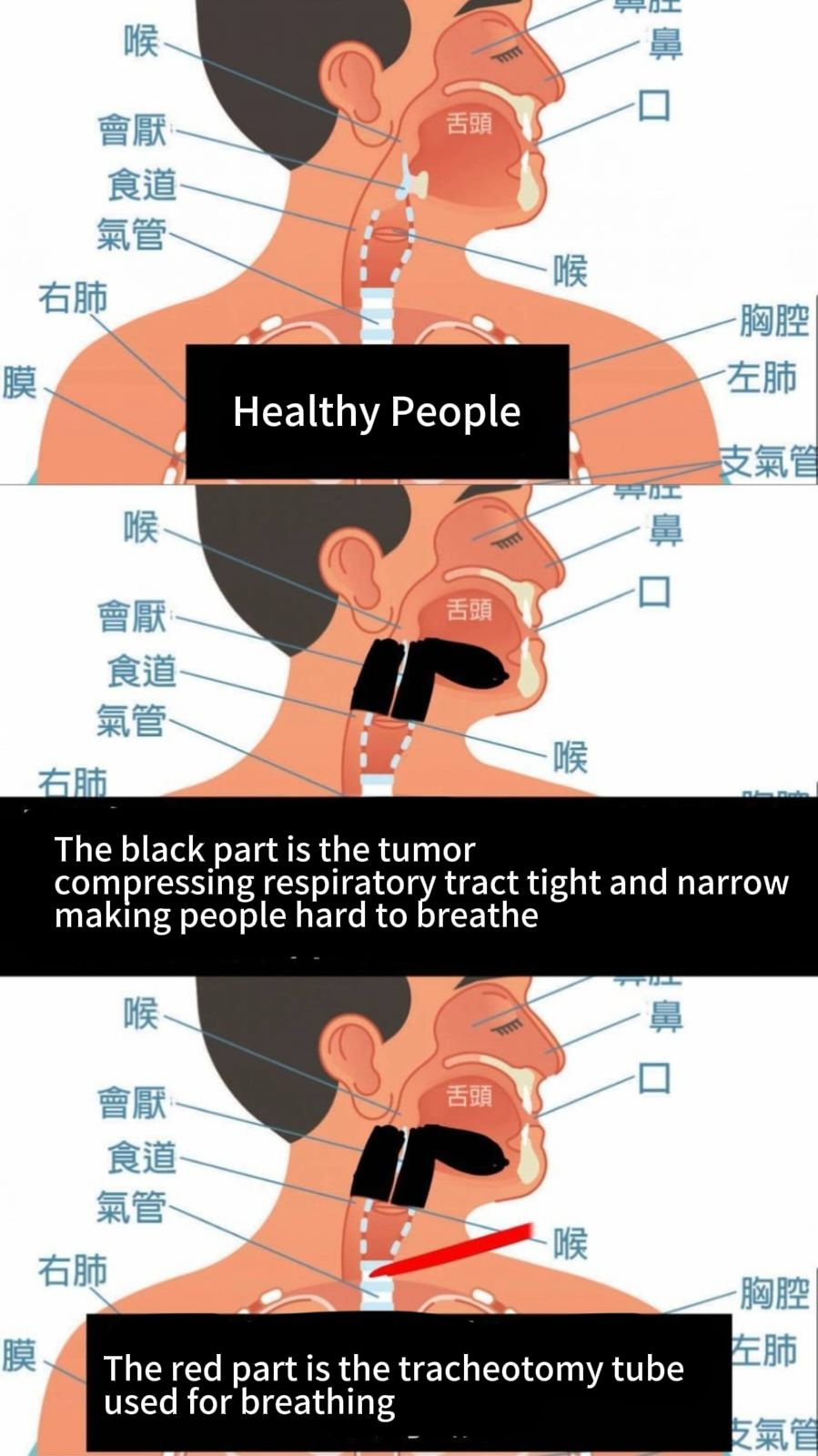
The final video was a blend of visuals and sound, perfectly encapsulating the essence of our blog. Key moments like the explanation of palliative care, tracheostomy, or aggressive treatment options were brought to life in a way that allowed viewers to feel the weight of the decisions.
Monterey Language Services explores the emotional and professional challenges medical interpreters face from navigating complex medical jargon to bearing the weight of traumatic situations.
Stay tuned as we continue exploring the boundaries of technology and storytelling, bringing more interpretation issues into the spotlight.